 
Some patients say they are helpful in the short-term but harmful in the long-term.Ĭurrently there are no established guidelines on how to stop taking antipsychotics, which is partly why psychiatrists are reluctant to do so. However, some people find the drugs do not help them or that the side effects (which can sometimes contribute to long term health complications) outweigh the benefits, while many people who then stop taking antipsychotics experience withdrawal effects, which can be severe**. These drugs are also increasingly prescribed for conditions like insomnia and anxiety ‘off-label’ (without being licensed for these conditions by the UK’s MHRA). Stopping medications is an important part of the job of a psychiatrist, yet it has received relatively little attention.”Īntipsychotics are one of the fastest growing classes of drugs being prescribed in England*, growing from 660,000 people (9.4 million prescriptions) in 2015/2016 to 750,000 people in 2019/2020.Īntipsychotics are often recommended life-long for people diagnosed with schizophrenia or other serious mental illnesses because they are effective at controlling psychotic symptoms in the short term and might reduce the risk of relapse. From my own experience I know how hard it can be to wean off psychiatric medications – so we set out to write guidance on how to withdraw safely from antipsychotics. Lead author Dr Mark Horowitz (UCL Psychiatry) said: “Surprisingly, there are no published guidelines on how to come off antipsychotics. Withdrawal symptoms can be severe, and may include psychotic symptoms similar to the underlying condition, which can result in patients being advised to remain on the medication indefinitely, even though the new symptoms might have been avoidable with a carefully-managed withdrawal. The review, published in Schizophrenia Bulletin, is the first ever scientific paper outlining how exactly antipsychotic medication should be reduced in order to minimise both withdrawal effects and the risk of relapse. People taking Risperidone for schizophrenia more commonly experience insomnia, while those taking it for bipolar mania are more likely to experience tiredness.Withdrawing from antipsychotics may require months or even years, and patients need to gradually reduce to very low doses, according to a new analysis led by UCL and King’s College London academics. Risperidone (Risperdal) - has been known to cause both tiredness and insomnia depending on the individual.Aripiprazole (Abilify) - sedation is a common side effect.Olanzapine (Zyprexa) - sedation is a common side effect.Quetiapine (Seroquel) - known for extreme sedation and sometimes prescribed for anxiety or sleep disorders.Tolerance to the sedating effect of these drugs may develop during treatment and withdrawal may result in insomnia.Ĭommonly prescribed atypical antipsychotics include: 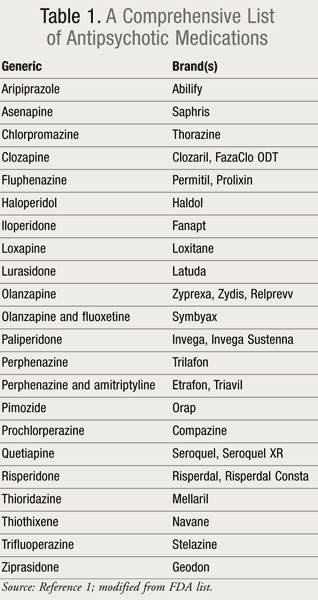
The atypical, or second generation, antipsychotics are less prone to inducing sedation although some atypical antipsychotic drugs are still associated with extreme tiredness and may shift sleep patterns. Chlorpromazine - known for both extreme sedation and anti-anxiety properties.Tolerance to the sedating effect of these drugs may develop during treatment.Įxamples of typical antipsychotics include: Sleep cycles, including REM-sleep, are not altered by antipsychotics, although total sleep time may increase. Typical antipsychotic medications also tend to decrease muscular actions created by psychiatric disorders, like anxiety and obsessive-compulsive disorder, which also may improve sleep. Most typical, or first-generation, antipsychotics have sedating effects. How sedating an antipsychotic is depends on dose and type. Read more about antipsychotic medications and sleep disorders.Īntipsychotics are also known as major tranquilizers and are sometimes used to treat sleep disorders due to their sedating effects. Low doses of antipsychotic medications are prescribed to treat sleep disorders like insomnia. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
